CAR-T cells have been developed as adoptive anti-tumor immunotherapy in recent years. The principle is to use of genetic engineering techniques to acquire T cells from cancer patients in vitro, the patient's T cells can be genetically modified to stably express antibodies on their surface, then abundantly cultivating CAR-T cells in vitro and reinfused into the patient's. CAR-T cells mostly used in curing hematologic tumors and malignant solid tumors, including breast, cervical, lung, liver and stomach cancer and so on .
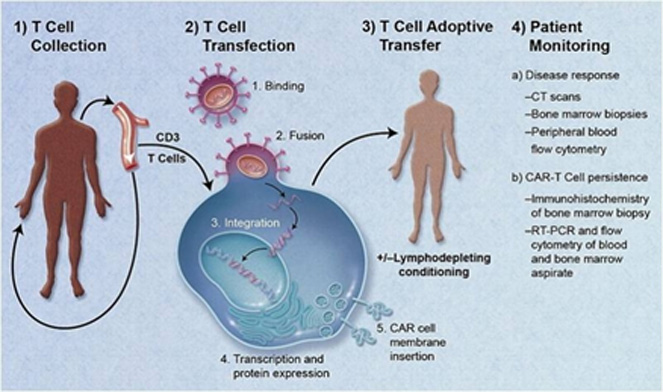
CAR-T cells Immunotherapy have divided into five operations: first, autologous T cells are separated from the patient's blood; second, genes encoded to recognize cancer cells are transferred into the patient's T cells using an inactive virus called a viral vector; third, abundantly cultivating CAR-T cells in vitro; fourth, the modified T cells are reinfused into the patient's blood; fifth, monitor the patient's response.
More therapeutic accuracy. CAR can specifically recognize tumor-associated antigens without restriction of MHC and immune evasion.
More multi-targeted. Both protein antigens and glycolipid antigens can be used as target antigens to expand treatment coverage.
More extensive tumor killing. In view of many tumor cells express the same tumor antigen, once CAR gene construction for a tumor antigen is completed, which is widely used.
More persistence tumor killing. CAR contains additional co-stimulatory signals, which promoted T cells' proliferation and survival time, and can resist the local immune suppression microenvironment.